|
In this blog, we will explore the significance of dental cleanings and how often you should get them. Maintaining good oral hygiene is essential for overall health, and how regularly should you get your teeth cleaned? play a vital role in achieving it. Let's delve into the topic and understand the importance of scheduling dental cleanings.
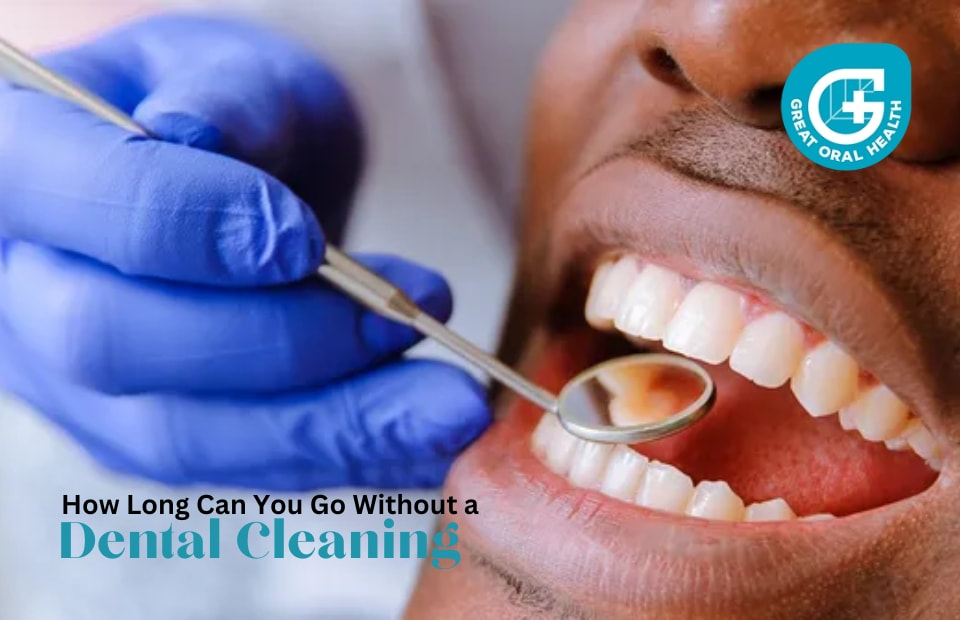
Importance of Dental Cleanings Regular dental cleanings are crucial for preventing various oral health issues such as cavities, gum disease, and bad breath. Professional cleanings help remove plaque and tartar buildup, which are often missed during regular brushing and flossing. This process not only keeps your teeth and gums healthy but also enhances your smile. Frequency of Dental Cleanings The frequency of dental cleanings depends on various factors, including individual oral health, age, and lifestyle habits. Most dentists recommend biannual cleanings for the average person with good oral hygiene. However, some individuals may require more frequent cleanings due to specific conditions. Factors Affecting Dental Cleaning Intervals Several factors influence how often you should get a dental cleaning. These include genetics, diet, tobacco use, existing oral health conditions, and dental habits. Your dentist will assess these factors to determine the appropriate cleaning schedule tailored to your needs. Read More About: How To Choose The Best Toothpaste For Strong Teeth And Gums: Signs That You Need a Dental Cleaning Apart from the recommended schedule, certain signs indicate that you should schedule a dental cleaning sooner. These signs may include persistent bad breath, swollen or bleeding gums, tooth sensitivity, or visible tartar buildup on your teeth. What Happens During a Dental Cleaning? A dental cleaning involves various steps to ensure your teeth and gums are thoroughly cleaned. Dental professionals use specialized tools to remove plaque, tartar, and stains from your teeth. They also perform a comprehensive examination to detect any potential oral health issues. Benefits of Regular Dental Cleanings Regular dental cleanings offer numerous benefits, such as preventing cavities and gum disease, reducing the risk of tooth loss, and enhancing the appearance of your smile. Additionally, maintaining good oral health contributes to overall well-being. Dental Cleaning for Children Children should start visiting the dentist for regular cleanings as soon as their first tooth erupts. Early dental visits help children become comfortable with dental care and establish a strong foundation for their oral health. Dental Cleaning for Adults Adults with good oral hygiene can benefit from biannual dental cleanings to maintain healthy teeth and gums. These cleanings are essential for preventing oral health issues and detecting any potential problems early. Dental Cleaning for Seniors As we age, oral health becomes even more critical. Seniors should continue with regular dental cleanings to ensure healthy teeth and gums and prevent issues associated with aging. Dental Cleaning for Pregnant Women Pregnancy can lead to various oral health changes, making dental cleanings vital during this time. Proper dental care during pregnancy can help prevent issues like pregnancy gingivitis and ensure a healthy pregnancy. Dental Cleaning and Overall Health Maintaining good oral health has implications beyond your mouth. Studies have shown links between oral health and overall health, with poor oral hygiene being associated with certain systemic conditions. Tips for Maintaining Good Oral Hygiene Apart from regular dental cleanings, practicing good oral hygiene at home is essential. This includes brushing twice a day, flossing daily, maintaining a healthy diet, and avoiding tobacco products. Conclusion In conclusion, regular dental cleanings are a cornerstone of maintaining good oral health. The frequency of cleanings varies from person to person and depends on several factors. By following your dentist's recommendations and practicing good oral hygiene, you can enjoy a healthy smile and overall well-being.
0 Comments
The tongue is a remarkable organ that plays a crucial role in various essential functions of the human body. It is a muscular structure covered with a specialized type of tissue known as keratinized epithelium. In this article, we will explore the reasons behind the keratinization of the tongue and its significance in maintaining oral health and overall well-being.
Table of Contents
Structure and Function of the Tongue The tongue consists of muscles covered with a specialized type of tissue called mucosa. It is divided into regions known as the apex, body, and root. The surface of the tongue is covered with papillae, tiny bumps that contain taste buds responsible for our sense of taste. The Process of Keratinization Keratinization is the natural process by which epithelial cells in the outer layer of the skin, or in this case, the tongue, undergo transformation and become filled with keratin. Keratin is a tough, fibrous protein that provides strength and protection to the tissue. Reasons for Keratinization The keratinization of the tongue serves several important purposes. Firstly, it enhances the durability of the tongue, enabling it to withstand friction and mechanical stress during various activities such as chewing and speaking. Additionally, keratinization protects the tongue from injuries and potential infections. Read More About: What Is Keratinized Tissue And Why Is It Important In Dental Implants The Importance of Keratinized Epithelium in the Tongue The keratinized epithelium in the tongue is vital for maintaining oral health. It acts as a barrier, preventing harmful substances, such as bacteria and toxins, from entering the underlying tissues. Furthermore, the keratinized surface of the tongue aids in the formation of a seal with the palate, facilitating the creation of negative pressure necessary for proper suction during breastfeeding and swallowing. Factors Affecting Tongue Keratinization Several factors can influence the degree of keratinization in the tongue. Genetic predisposition, oral hygiene practices, overall health, and lifestyle choices such as smoking and alcohol consumption can impact the process. Proper nutrition, including an adequate intake of vitamins and minerals, also plays a significant role in maintaining a healthy and well-keratinized tongue. Maintaining a Healthy Keratinized Tongue To keep the tongue in optimal condition, it is important to practice good oral hygiene. Regular brushing of the tongue with a soft-bristled toothbrush or tongue scraper helps remove bacteria and debris. Adequate hydration, a balanced diet, and avoiding habits like smoking contribute to the overall health of the tongue. Common Tongue Conditions Certain conditions can affect the keratinized epithelium of the tongue, leading to discomfort and potential health issues. Some common tongue conditions include geographic tongue, hairy tongue, oral thrush, and glossitis. It is essential to seek professional dental care if any unusual symptoms or changes are observed in the tongue. Conclusion The tongue's keratinized epithelium plays a crucial role in maintaining oral health and ensuring the proper functioning of this versatile organ. Its keratinized surface provides protection, durability, and the ability to perform various essential functions. By understanding the process of keratinization and implementing good oral hygiene practices, we can maintain a healthy and well-functioning tongue.  Dental x-rays, also known as radiographs, play a crucial role in diagnosing dental conditions and planning appropriate treatment. They provide valuable insights into the underlying structures of teeth, gums, and jawbones, helping dentists identify issues that may not be visible during a regular dental examination. However, as with any form of medical imaging, it is essential to prioritize safety during the process to minimize radiation exposure risks. In this article, we will explore the safety procedures involved in taking dental x-rays to ensure the well-being of both patients and dental practitioners. Use of Lead Aprons and Collars: One of the fundamental safety measures in dental radiography is the use of lead aprons and collars. These protective garments are designed to absorb radiation and shield the patient's vital organs from unnecessary exposure. Lead aprons cover the torso, while lead collars provide protection to the thyroid gland, which is particularly sensitive to radiation. These lead shielding accessories are mandatory for all patients undergoing dental x-rays, regardless of their age or gender. Thyroid Collars for Children: When it comes to pediatric dental patients, extra caution is exercised due to their heightened sensitivity to radiation. In addition to the lead apron, a specialized thyroid collar is used to provide additional shielding to the thyroid gland. Children are more susceptible to radiation-related risks, and therefore, this extra protection is necessary to safeguard their long-term health. Explore More: What Are Dental X-Rays? Fast Film or Digital Imaging: Advancements in dental technology have provided alternative options for capturing dental x-rays. Traditional film-based radiography has largely been replaced by digital imaging systems, which offer numerous benefits, including reduced radiation exposure. Digital x-ray sensors require significantly less radiation to produce a high-quality image compared to traditional film. Additionally, digital images can be processed and viewed instantly, eliminating the need for film development and reducing waiting times for patients. Rectangular Collimation: Collimation refers to the process of restricting the x-ray beam to the specific area of interest. By using rectangular collimation instead of the older circular technique, the size of the x-ray beam is limited to the exact region being imaged. This precise targeting helps minimize unnecessary radiation exposure to surrounding areas, thus enhancing patient safety. Proper Positioning and Technique: Accurate positioning of the patient and proper technique during the dental x-ray procedure are crucial to obtain high-quality images while minimizing radiation exposure. Dental practitioners should ensure that the patient's head, body, and dental film or sensor are appropriately aligned to capture the necessary diagnostic information. Aiming for the correct angle and distance reduces the need for retakes and avoids unnecessary radiation exposure to the patient. Cone Beam Computed Tomography (CBCT) for Complex Cases: In cases where traditional dental x-rays do not provide sufficient information, Cone Beam Computed Tomography (CBCT) may be utilized. CBCT produces three-dimensional images of the patient's oral and maxillofacial structures. While CBCT involves a higher radiation dose than regular dental x-rays, it offers valuable information for complex cases such as impacted teeth, jaw pathology, or implant planning. Dental practitioners must weigh the benefits and risks of CBCT, ensuring that it is only employed when absolutely necessary. Monitoring Radiation Exposure: To ensure ongoing safety, dental practices should implement radiation monitoring protocols. Radiation dosimeters can be worn by dental professionals to monitor their exposure levels. Regular checks and evaluations are performed to ensure that staff members are not exceeding recommended radiation limits. Furthermore, dental practices must maintain accurate records of all patient radiographs, including the type of dentax-ray taken, the date, and any relevant details. This information enables dentists to track and limit radiation exposure, ensuring patient safety and complying with regulatory guidelines. Conclusion: Safety is paramount when it comes to dental x-rays. By following proper procedures and implementing safety measures, dental practitioners can minimize radiation exposure risks for both patients and themselves. The use of lead aprons, thyroid collars, digital imaging systems, rectangular collimation, and precise positioning techniques all contribute to enhancing safety. Additionally, dentists must exercise caution when considering the use of CBCT, reserving it for cases that require advanced imaging capabilities. Regular monitoring of radiation exposure and maintaining comprehensive records further promote safety and compliance. By prioritizing safety procedures, dental professionals can confidently provide accurate diagnoses and effective treatments while safeguarding the well-being of their patients.  Teeth are an integral part of our bodies, serving essential functions in the process of digestion and communication. However, when it comes to categorizing teeth as either an organ or a bone, the answer is not as straightforward as one might think. Teeth are unique structures that possess characteristics of both organs and bones. To better understand this distinction, it is important to delve into the nature of teeth, their composition, and their functions within the human body. First and foremost, let us explore the definition of an organ. An organ is a specialized structure made up of different tissues that work together to perform a specific function. When we think of organs, the heart, liver, lungs, and kidneys usually come to mind. These organs are composed of multiple types of tissues, such as muscle, connective tissue, and epithelial tissue. They have specific functions and work in coordination to maintain overall bodily functions. Read more: Are Your Teeth Bones On the other hand, bones are rigid structures that provide support, protection, and mobility to the body. They are made up of specialized connective tissues called bone tissue. Bones have a complex structure, consisting of a dense outer layer called cortical bone and a spongy inner layer known as trabecular bone. They also contain bone marrow, which is responsible for producing red and white blood cells. Now, let's examine teeth in light of these definitions. Teeth are hard, calcified structures embedded in the jawbones of the oral cavity. They are primarily composed of four different types of tissues: enamel, dentin, cementum, and pulp. Enamel is the outermost layer, the hardest substance in the human body, and is primarily made up of minerals. Dentin, the layer beneath the enamel, constitutes the bulk of the tooth and is similar to bone tissue in terms of composition. Cementum covers the roots of the tooth and aids in anchoring it to the jawbone. Lastly, the pulp is the innermost part, containing nerves, blood vessels, and connective tissues. Based on this information, it becomes evident that teeth do not meet the criteria of a typical organ. They lack the diverse range of tissues found in organs like the heart or liver. However, teeth are not purely bone structures either, as they possess distinct components like enamel, dentin, cementum, and pulp that set them apart from bones. Although teeth do not fit the conventional definition of an organ, they are vital for multiple bodily functions. The primary function of teeth is to break down food mechanically through chewing, which initiates the process of digestion. Without teeth, our ability to consume a wide variety of foods and extract nutrients from them would be severely compromised. Teeth also play a crucial role in speech, enabling us to articulate sounds correctly and communicate effectively. Explore More: What are teeth made of Moreover, teeth contribute to maintaining the structure and integrity of the jawbone. The roots of the teeth are embedded within the alveolar sockets of the jawbone, providing support and preventing the collapse of the facial structure. The presence of teeth stimulates the bone tissue, promoting bone density and preventing bone loss. When teeth are lost or extracted, the underlying jawbone can begin to deteriorate over time due to lack of stimulation. In conclusion, teeth can be considered unique structures that possess characteristics of both organs and bones. While they do not meet the definition of a traditional organ due to their limited tissue composition, they perform vital functions and contribute significantly to our overall well-being. Teeth enable us to chew and digest food properly, play a role in speech, and help maintain the integrity of the jawbone. Understanding the complex nature of teeth is crucial for appreciating their importance and taking proper care of them through regular dental hygiene and professional dental care. Enamel loss, also known as tooth enamel erosion, can be a concerning dental issue. The enamel is the protective outer layer of your teeth, and when it erodes, it exposes the underlying layers, increasing the risk of sensitivity, decay, and other oral problems. In this article, we will explore the effects of enamel loss and whether it is permanent. Table of Contents
Introduction Tooth enamel is the hardest substance in the human body, but it can still wear away over time due to various factors. Understanding the implications of enamel loss and its potential reversibility can help you take proactive steps to protect your oral health. Understanding Enamel Loss Enamel loss refers to the gradual wearing away of the tooth enamel, which can lead to thinner and weaker teeth. The enamel protects the underlying dentin and pulp, and its erosion exposes these sensitive areas, making the teeth more vulnerable to decay, sensitivity, and other issues. Causes of Enamel Loss Enamel loss can occur due to several factors, including:
Effects of Enamel Loss Enamel loss can have various effects on your teeth, including:
Can Enamel Loss Be Reversed? Unfortunately, once the enamel is lost, it cannot regenerate or repair itself. Enamel is a non-living tissue, and the body does not have the ability to replace it. However, early-stage enamel erosion can be halted and further progression can be prevented through proper dental care and lifestyle adjustments. Preventing Enamel Loss While enamel loss may be irreversible, you can take steps to prevent further erosion and protect your remaining enamel:
Conclusion Enamel loss is a serious dental concern that can have long-term effects on your oral health. While it is not possible to regenerate lost enamel, you can prevent further erosion and protect your remaining enamel through proper dental care and lifestyle choices. Regular dental check-ups and professional cleanings are also crucial for detecting and addressing enamel loss in its early stages. When it comes to replacing missing teeth, there are various options available, and two common choices are dental bridges and dental implants. Both options have their own advantages and considerations. In this article, we will explore the differences between bridges and implants to help you make an informed decision about which option may be better for you.
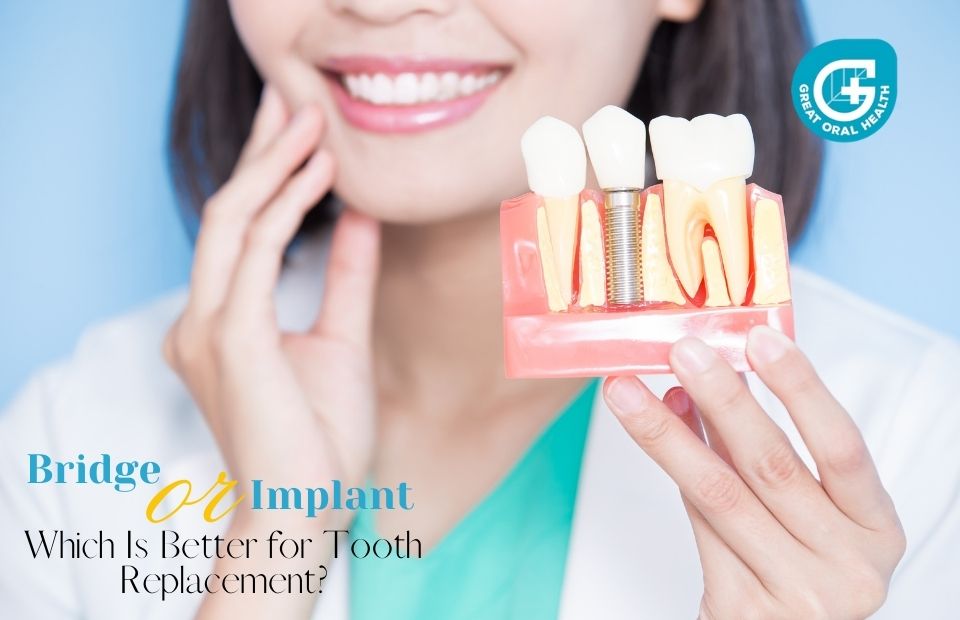
Table of Contents Introduction Replacing missing teeth is essential not only for restoring your smile but also for maintaining oral health and function. Dental bridges and implants are popular solutions for replacing missing teeth, and the decision between the two depends on several factors, including your oral health, personal preferences, and budget. Dental Bridges Dental bridges are prosthetic devices that bridge the gap created by missing teeth. They consist of artificial teeth (pontics) held in place by dental crowns on the adjacent teeth, which serve as anchors. Bridges are typically made from materials such as porcelain or ceramic fused to metal. They offer several advantages, including:
Discover More: 101 Guide To What Is A Dental Implant Dental Implants Dental implants are titanium posts that are surgically placed into the jawbone to replace the root of a missing tooth. Once the implant integrates with the bone, a dental crown is attached to the implant, providing a natural-looking and functional replacement tooth. Implants offer several advantages, including:
Factors to Consider To determine which option is better for you, consider the following factors:
Discover More: What Is The Latest Technology In Dentistry? Conclusion The decision between a dental bridge and implant depends on various factors, and it's important to consult with your dentist to assess your specific situation. Dental bridges are a reliable and cost-effective option for replacing missing teeth, while dental implants offer a more permanent and natural solution. Consider your oral health, long-term goals, aesthetics, and budget when making a decision. Your dentist will guide you in selecting the best option to restore your smile and oral function. Autoimmune diseases are conditions in which the body's immune system mistakenly attacks its own healthy cells and tissues. While these diseases can affect various organs and systems, some specifically target the teeth and gums, leading to oral health problems. In this article, we will explore autoimmune diseases that can affect teeth and gums and discuss how does autoimmune disease affect oral health?
Table of Contents
Introduction Autoimmune diseases arise when the immune system malfunctions and starts attacking healthy tissues. When these diseases affect the oral cavity, they can cause inflammation, damage, and other complications that impact the teeth and gums. Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease primarily affecting the joints. However, it can also cause oral manifestations, including gum inflammation (gingivitis) and periodontitis. These conditions can lead to gum recession, tooth loss, and difficulties in chewing and speaking. Additionally, certain medications used to treat RA can increase the risk of oral health problems. Systemic Lupus Erythematosus (SLE) Systemic Lupus Erythematosus, commonly known as lupus, is a chronic autoimmune disease that can affect multiple organs, including the oral cavity. Oral symptoms of SLE may include oral ulcers, oral pain, and gum inflammation. These symptoms can contribute to difficulties in maintaining proper oral hygiene and may require tailored dental care. Enhance Your Knowledge: Is Gum Health Reversible? You Must Know Today Sjögren's Syndrome Sjögren's syndrome is an autoimmune disorder characterized by the immune system attacking the moisture-producing glands, leading to dryness of the mouth and eyes. The lack of saliva in the mouth can increase the risk of dental decay, gum disease, and oral infections. It can also cause oral discomfort, difficulties in speaking and swallowing, and challenges with wearing dentures. Behçet's Disease Behçet's disease is a rare autoimmune condition that causes inflammation of blood vessels throughout the body. It can affect the oral cavity, leading to symptoms such as mouth ulcers, gingivitis, and oral pain. These oral manifestations can impact oral hygiene practices and require specialized dental care. Conclusion Autoimmune diseases such as rheumatoid arthritis, systemic lupus erythematosus (SLE), Sjögren's syndrome, and Behçet's disease can have a significant impact on oral health by affecting the teeth and gums. It is important for individuals with these conditions to work closely with their healthcare team, including dentists, to manage oral symptoms, maintain good oral hygiene, and seek appropriate treatment. Regular dental check-ups, proper oral care, and early intervention can help minimize the impact of these autoimmune diseases on teeth and gums. Bleeding gums can be an indication of various underlying oral health issues, and it doesn't necessarily mean that a person is not flossing. In fact, bleeding gums can occur even if someone is practicing proper flossing habits. In this article, we will explore the reasons why do my gums bleed when i floss? Or may this occur despite regular flossing.
Table of Contents Introduction Bleeding gums can be a cause for concern and may indicate an underlying oral health problems. However, it's important to note that bleeding gums don't automatically mean that a person is not flossing. Let's explore the possible causes of bleeding gums. Causes of Bleeding Gums Several factors can contribute to bleeding gums, including:
Importance of Flossing Flossing plays a crucial role in maintaining optimal oral hygiene. It helps remove plaque, bacteria, and food particles from between the teeth and along the gumline. Regular flossing can prevent gum disease, tooth decay, and bad breath. Addressing Bleeding Gums If you experience bleeding gums, even with regular flossing, consider the following steps:
Conclusion Bleeding gums can occur due to various factors, including gum disease, hormonal changes, medications, vitamin deficiencies, and systemic conditions. It's important to understand that bleeding gums do not necessarily indicate a lack of flossing. Regular flossing, along with proper oral hygiene practices and professional dental care, can help maintain healthy gums and overall oral health. Understanding the crossbite problem is essential to address this common dental issue effectively. In this article, we will explore the definition, types, causes, and potential complications associated with crossbite. Let's delve into the world of crossbite and gain insights into this oral condition.
Table of Contents
Introduction The crossbite problem refers to a misalignment of the upper and lower teeth when biting down. This malocclusion can lead to functional and aesthetic concerns, making it crucial to understand its causes and seek appropriate treatment. Definition of Crossbite Crossbite occurs when the upper teeth are positioned inside the lower teeth upon biting. It can affect a single tooth or multiple teeth, and it can occur at the front or back of the mouth. This misalignment can result in an uneven bite and potential oral health complications. Types of Crossbite Crossbite can be classified into two main types: - Posterior Crossbite Posterior crossbite refers to the misalignment of the back teeth (molars and premolars). In this case, the upper teeth fit inside the lower teeth when biting down, causing an incorrect bite relationship. - Anterior Crossbite Anterior crossbite involves the misalignment of the front teeth (incisors). The upper incisors sit behind the lower incisors when biting, leading to an abnormal bite pattern. Read More: Types Of Teeth, Their Function And Shapes Causes of Crossbite Several factors contribute to the development of a crossbite. The common causes include: - Genetics: Genetic factors play a role in determining the size and shape of the jaw. If a family member has a crossbite, there is a higher likelihood of inheriting this malocclusion. - Jaw Irregularities: Irregularities in jaw growth can result in a crossbite. These irregularities can be influenced by genetic factors, childhood habits, or certain medical conditions. - Childhood Habits: Prolonged thumb sucking, pacifier use, or other oral habits beyond a certain age can impact the development of the teeth and jaws, leading to crossbite. - Premature Tooth Loss: The premature loss of baby teeth can disrupt the natural alignment process of permanent teeth. This disruption may contribute to the development of crossbite if adjacent teeth drift into the empty space. - Dental Habits: Certain dental habits, such as tongue thrusting or prolonged bottle feeding, can affect the position of the teeth and jaws, leading to a crossbite. Complications of Crossbite If left untreated, crossbite can lead to several complications, including:
Diagnosis and Treatment Diagnosing crossbite involves a comprehensive dental examination, including bite analysis and dental X-rays. Treatment options vary depending on the severity of the crossbite and may include:
Preventive Measures Taking preventive measures can help reduce the risk of developing a crossbite. Strategies include:
Conclusion Understanding the crossbite problem is essential for maintaining optimal oral health. Genetic factors, jaw irregularities, childhood habits, premature tooth loss, and dental habits contribute to the development of a crossbite. Early diagnosis and appropriate treatment can prevent complications and ensure proper dental alignment. Regular dental check-ups and timely intervention are crucial for effective management of crossbite.  Gingivitis is a common dental condition characterized by inflammation of the gums. It is caused by the buildup of plaque, a sticky film of bacteria that forms on the teeth and gums. If left untreated, gingivitis can progress into a more severe form of gum disease known as periodontitis. Therefore, it is important to address gingivitis early on and seek appropriate treatment. Introduction Gingivitis is a reversible form of gum disease that affects people of all ages. It is primarily caused by poor oral hygiene, which leads to the accumulation of plaque and tartar on the teeth and gum line. The good news is that gingivitis can be effectively treated, especially when addressed in its early stages. Understanding Gingivitis Gingivitis is characterized by red, swollen, and tender gums. Other common symptoms include bleeding while brushing or flossing, bad breath, and gum recession. If you notice any of these signs, it is essential to consult with a dentist for a proper diagnosis and treatment plan. Importance of Early Treatment Treating gingivitis early is crucial to prevent its progression into periodontitis, a more severe form of gum disease that can result in tooth loss and other complications. The first-line treatment for gingivitis focuses on eliminating the underlying cause, reducing inflammation, and promoting gum health. Professional Dental Cleaning Professional dental cleaning, also known as scaling and root planing, is an essential step in the treatment of gingivitis. This procedure involves the removal of plaque and tartar from the teeth and beneath the gum line. It helps eliminate the bacteria that cause inflammation and allows the gums to heal. Improving Oral Hygiene Practices To effectively manage gingivitis, it is vital to establish and maintain good oral hygiene practices. This includes brushing and flossing daily to remove plaque and food particles from the teeth and gums. Proper Brushing Technique Using a soft-bristled toothbrush, gently brush your teeth at least twice a day. Pay attention to the gum line and brush in a circular motion to remove plaque effectively. It is also important to replace your toothbrush every three to four months or sooner if the bristles become frayed. Flossing and Interdental Cleaning Flossing plays a crucial role in gingivitis treatment as it helps remove plaque and debris from areas that a toothbrush cannot reach. Make sure to floss between each tooth and along the gumline. Additionally, interdental brushes or water flossers can be used to clean between teeth and massage the gums. Antimicrobial Mouthwash Using an antimicrobial mouthwash can further aid in the treatment of gingivitis. These mouthwashes contain ingredients that target and kill the bacteria responsible for gum inflammation. Rinse your mouth with the antimicrobial mouthwash after brushing and flossing. This will help reach areas that may have been missed during brushing and reduce the bacteria that contribute to gingivitis. Swish the mouthwash around your mouth for the recommended duration stated on the product label, ensuring that it reaches all areas of your gums and teeth. Spit out the mouthwash after rinsing and avoid eating or drinking anything for at least 30 minutes to allow the active ingredients to work effectively. Read More: How is Gingivitis Diagnosed? Balanced Diet and Lifestyle Changes Maintaining a balanced diet and making certain lifestyle changes can significantly contribute to the treatment of gingivitis. A healthy diet rich in fruits, vegetables, whole grains, and lean proteins provides essential nutrients for gum health. Avoiding sugary foods and beverages is also beneficial as they can contribute to plaque formation. Additionally, drinking plenty of water helps stimulate saliva production, which naturally helps cleanse the mouth and reduce bacteria. Quitting Smoking Smoking has detrimental effects on oral health, including an increased risk of gum disease. Quitting smoking is not only beneficial for your overall health but also plays a vital role in the treatment of gingivitis. By quitting smoking, you can reduce inflammation in the gums and improve the chances of successful treatment. Stress Management Stress can affect your oral health as well. High-stress levels can weaken the immune system, making it harder for your body to fight off infections, including gum disease. Implementing stress management techniques such as exercise, meditation, and engaging in activities you enjoy can help reduce stress and improve your oral health. Regular Dental Check-ups Regular dental check-ups are crucial for the early detection and treatment of gingivitis. Dentists can assess the condition of your gums, provide professional cleaning, and offer personalized recommendations for your oral hygiene routine. It is recommended to visit your dentist at least twice a year or as advised by your oral healthcare professional. Home Remedies for Gingivitis While professional dental care is essential, there are also some home remedies that can complement the treatment of gingivitis. These remedies include rinsing with a saltwater solution, applying aloe vera gel to the gums, using hydrogen peroxide mouthwash (diluted with water), and applying cold compresses to reduce gum inflammation. However, it is important to note that these home remedies should not replace professional dental care but can provide temporary relief and support gum health. Conclusion In conclusion, the first-line treatment for gingivitis involves a comprehensive approach to address the underlying causes of gum inflammation. Professional dental cleaning, improved oral hygiene practices, antimicrobial mouthwash, a balanced diet, lifestyle changes, stress management, and regular dental check-ups are essential in managing and preventing the progression of gingivitis. By taking proactive steps and seeking timely treatment, you can maintain optimal oral health and prevent the complications associated with gum disease. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
June 2023
Categories |




 RSS Feed
RSS Feed
