 Teething is a milestone that every child goes through, but it can be a challenging time for both babies and parents. The eruption of those tiny pearly whites can cause a range of symptoms that may vary from child to child. In this comprehensive guide, we will explore the factors that contribute to teething symptoms and provide helpful insights on how to manage them effectively. Introduction Teething is a natural process that occurs when a baby's teeth start to emerge through the gums. This typically begins around six months of age, although it can vary. As the teeth push through the gum tissue, it can cause discomfort and a variety of symptoms that may make your little one irritable and fussy. Understanding the causes behind these symptoms can help parents provide the necessary care and comfort for their teething baby. Expand your Knowledge What is a teething syndrome? What Causes Teething Symptoms? Teething symptoms are primarily caused by the physical process of the teeth breaking through the gum line. The pressure exerted by the emerging teeth can cause inflammation, irritation, and discomfort. Here are some key factors that contribute to teething symptoms:
1: When do teething symptoms typically start? Teething symptoms can begin as early as three months of age, but most babies start teething around six months. However, it's essential to remember that each baby is different, and the timing can vary. 2: How long do teething symptoms last? Teething symptoms can last for several days or weeks, depending on the individual child. Once the tooth has fully emerged through the gum line, the symptoms usually subside.
0 Comments
 Introduction Taking care of our teeth is essential for maintaining good oral health. One common concern many people have is how to naturally fix their tooth enamel. Tooth enamel is the protective outer layer of our teeth that helps prevent tooth decay and sensitivity. Over time, enamel can become damaged due to various factors such as acidic foods, poor oral hygiene, and teeth grinding. In this article, we will explore natural ways to improve and restore tooth enamel to promote healthy teeth and a beautiful smile. Why is Tooth Enamel Important? Before diving into natural remedies, it's crucial to understand the importance of tooth enamel. Tooth enamel is the hardest substance in the human body, even stronger than bone. It acts as a shield, protecting the sensitive inner layers of the teeth from decay-causing bacteria, acids, and temperature changes. When enamel erodes or weakens, it exposes the underlying dentin, making the teeth more susceptible to cavities, discoloration, and sensitivity. How Can I Fix My Tooth Enamel Naturally? 1. Maintain Good Oral Hygiene One of the fundamental steps in preserving tooth enamel is to maintain good oral hygiene practices. This includes: Brushing your teeth twice a day using a soft-bristled toothbrush and fluoride toothpaste. Flossing daily to remove plaque and food particles from between your teeth. Using a fluoride mouthwash to strengthen enamel and fight against bacteria. Avoid aggressive brushing, as it can wear down enamel over time. By following these simple habits, you can keep your tooth enamel strong and healthy. 2. Minimize Acidic Food and Drink Consumption Acidic foods and beverages can erode tooth enamel, so it's important to limit their consumption. Examples of acidic foods and drinks include citrus fruits, tomatoes, carbonated drinks, and fruit juices. When you do indulge in these foods, consider using a straw to minimize contact with your teeth and rinse your mouth with water afterward. 3. Increase Calcium and Vitamin D Intake Calcium and vitamin D play a crucial role in maintaining strong and healthy teeth. Calcium helps strengthen tooth enamel, while vitamin D aids in the absorption of calcium. Including calcium-rich foods in your diet, such as dairy products, leafy greens, and almonds, can help support enamel health. Additionally, spending time outdoors to get natural sunlight exposure or considering a vitamin D supplement can be beneficial. 4. Chew Sugar-Free Gum Chewing sugar-free gum, particularly one that contains xylitol, can stimulate saliva production. Saliva acts as a natural mouthwash, helping to neutralize acids and remineralize tooth enamel. However, it's important to note that excessive gum chewing can lead to jaw problems, so moderation is key. 5. Drink Plenty of Water Staying hydrated is not only good for your overall health but also for your teeth. Drinking plenty of water helps rinse away food particles and neutralize harmful acids, promoting a healthy oral environment. Opt for fluoridated water, when possible, as fluoride strengthens tooth enamel and helps prevent tooth decay. 6. Avoid Teeth Grinding and Clenching Teeth grinding, also known as bruxism, can wear down tooth enamel over time. If you suspect you grind or clench your teeth, especially during sleep, consider wearing a mouthguard. A custom-fitted mouthguard can help Protect your teeth from the damaging effects of grinding and clenching. Read More: How to Strengthen Tooth Enamel Naturally? In conclusion, taking care of our tooth enamel is essential for maintaining good oral health. While there is no magical solution to completely restore tooth enamel once it has been damaged, there are several natural remedies and lifestyle changes that can help improve its strength and prevent further erosion. By following good oral hygiene practices, minimizing acidic food and drink consumption, increasing calcium and vitamin D intake, chewing sugar-free gum, drinking plenty of water, and avoiding teeth grinding, we can promote the health and longevity of our tooth enamel.  Autoimmune diseases are a group of conditions where the immune system mistakenly attacks healthy cells in the body, causing inflammation and damage. These diseases can affect various organs and systems, leading to a wide range of symptoms. In this article, we will explore the 10 most common autoimmune diseases, their symptoms, causes, and available treatments. Introduction Autoimmune diseases are a significant health concern worldwide, affecting millions of people. They often result from a combination of genetic and environmental factors. While there are more than 80 different autoimmune diseases identified, some are more prevalent than others. Understanding the most common autoimmune diseases can help individuals recognize symptoms early and seek appropriate medical care. 10 Most Common Autoimmune Diseases? 1. Rheumatoid Arthritis (RA) Rheumatoid arthritis is a chronic inflammatory disease that primarily affects the joints, causing pain, swelling, and stiffness. It occurs when the immune system mistakenly attacks the synovium, the lining of the joints. RA can also affect other organs, such as the heart and lungs. Symptoms: Joint pain, swelling, morning stiffness, fatigue. Causes: Genetic predisposition, environmental factors, hormonal imbalances. Treatment: Medications (NSAIDs, DMARDs), physical therapy, lifestyle changes. 2. Systemic Lupus Erythematosus (SLE) Systemic lupus erythematosus, commonly known as lupus, is a chronic autoimmune disease that can affect multiple organs, including the skin, joints, kidneys, heart, and brain. Lupus is characterized by periods of flare-ups and remission. Symptoms: Fatigue, joint pain, rash, fever, hair loss. Causes: Genetic predisposition, hormonal factors, environmental triggers. Treatment: Medications (corticosteroids, immunosuppressants), lifestyle modifications. 3. Multiple Sclerosis (MS) Multiple sclerosis is a chronic neurological disorder in which the immune system mistakenly attacks the protective covering of nerve fibers in the central nervous system. This damage disrupts the flow of electrical impulses between the brain and the body. Symptoms: Fatigue, muscle weakness, difficulty walking, vision problems. Causes: Genetic susceptibility, and environmental factors. Treatment: Medications (immunomodulators, corticosteroids), physical therapy. 4. Type 1 Diabetes Type 1 diabetes is an autoimmune disease that occurs when the immune system destroys the insulin-producing cells in the pancreas. Without sufficient insulin, the body cannot regulate blood sugar levels effectively. Symptoms: Increased thirst, frequent urination, unexplained weight loss. Causes: Genetic predisposition, environmental triggers. Treatment: Insulin therapy, blood sugar monitoring, and lifestyle adjustments. Read More: Autoimmune Disease the Impact on your oral health 5. Celiac Disease Celiac disease is an autoimmune disorder triggered by the consumption of gluten, a protein found in wheat, barley, and rye. In individuals with celiac disease, gluten damages the lining of the small intestine, impairing nutrient absorption. Symptoms: Abdominal pain, bloating, diarrhea, weight loss. Causes: Genetic predisposition, gluten consumption. Treatment: Strict gluten-free diet, and nutritional support. 6. Psoriasis Psoriasis is a chronic autoimmune skin disorder characterized by the rapid overproduction of skin cells, leading to the formation of red, raised patches with silvery scales. It often causes itching and can also affect the joints, leading to joint pain. Symptoms: Red, raised patches, silvery scales, itching, and joint pain. Causes: Genetic predisposition, environmental factors, immune system dysfunction. Treatment: Topical creams, phototherapy, systemic medications. 7. Hashimoto's Thyroiditis Hashimoto's thyroiditis is an autoimmune condition where the immune system attacks the thyroid gland, resulting in chronic inflammation. This leads to an underactive thyroid (hypothyroidism) and can cause a range of symptoms. Symptoms: Fatigue, weight gain, sensitivity to cold, depression. Causes: Genetic predisposition, environmental triggers. Treatment: Thyroid hormone replacement therapy. 8. Graves' Disease Graves' disease is an autoimmune disorder characterized by an overactive thyroid gland (hyperthyroidism). The immune system produces antibodies that stimulate the thyroid gland to produce excessive amounts of thyroid hormone. Symptoms: Rapid heartbeat, weight loss, tremors, anxiety. Causes: Genetic predisposition, and environmental factors. Treatment: Medications (antithyroid drugs, beta-blockers), radioactive iodine therapy, surgery. 9. Inflammatory Bowel Disease (IBD) Inflammatory bowel disease refers to a group of conditions, including Crohn's disease and ulcerative colitis, that cause chronic inflammation in the digestive tract. These autoimmune disorders can lead to various gastrointestinal symptoms and complications. Symptoms: Abdominal pain, diarrhea, rectal bleeding, weight loss. Causes: Genetic susceptibility, environmental factors, immune system dysfunction. Treatment: Medications (anti-inflammatory drugs, immunosuppressants), dietary changes, surgery (in severe cases). Discover More: How Can Teeth Affect Your Sleep Quality 10. Sjögren's Syndrome Sjögren's syndrome is an autoimmune disorder primarily affecting the salivary and tear glands, resulting in dry eyes and mouth. It can also affect other parts of the body, including joints and organs. Symptoms: Dry eyes, dry mouth, joint pain, fatigue. Causes: Genetic predisposition, hormonal factors, viral infections. Treatment: Symptomatic relief (artificial tears, saliva substitutes), medications (anti-inflammatory drugs, immunosuppressants). These are the ten most common autoimmune diseases. It's important to note that while these conditions share autoimmune characteristics, their specific symptoms, causes, and treatments may vary. If you suspect you may have an autoimmune disease, it's crucial to consult with a healthcare professional for proper diagnosis and treatment. FAQs About Autoimmune Diseases Are autoimmune diseases hereditary? While there is a genetic component to autoimmune diseases, not all individuals with a family history of autoimmune conditions will develop the same disease. Genetic predisposition, combined with environmental triggers, contributes to the development of autoimmune diseases. Can stress trigger autoimmune diseases? Stress can potentially worsen symptoms in individuals with autoimmune diseases, but it is not a direct cause of these conditions. Stress management techniques and a healthy lifestyle may help alleviate symptoms.  Introduction Dental implants have revolutionized the field of dentistry, providing a long-lasting and aesthetically pleasing solution for missing teeth. Unlike traditional dentures or bridges, dental implants offer numerous benefits that improve oral health, functionality, and overall well-being. In this article, we will explore the advantages of using dental implants and why they are considered the gold standard for tooth replacement. What are Dental implants? One of the best ways to replace a tooth when you have lost bone is with a dental implant. This is usually a titanium post that is put into your jawbone and works as an anchor in place of the tooth root. The titanium root is then used to hold tooth prosthetics like dentures, crowns, and bridges in place. Most of the time, it is the best and most effective way to replace lost teeth because they are strong and can also hold false teeth. Read More: Different Types of dental implants The Remarkable Benefits of Dental Implants Improved Oral Functionality: Dental implants restore full chewing power, allowing you to enjoy your favorite foods without discomfort or limitations. With their strong foundation, implants provide stability similar to natural teeth, ensuring efficient biting and chewing. 1. Enhanced Aesthetic Appeal: One of the significant advantages of dental implants is their ability to replicate the appearance of natural teeth. Implants are custom-designed to match the shape, color, and alignment of your existing teeth, resulting in a seamless and beautiful smile. 2. Long-Term Durability: Unlike other tooth replacement options, dental implants are built to last. Made from biocompatible materials such as titanium, implants fuse with the jawbone through a process called osseointegration, creating a durable and permanent solution. 3. Preservation of Bone Structure: When a tooth is lost, the underlying jawbone may deteriorate over time due to a lack of stimulation. Dental implants mimic the function of natural tooth roots, stimulating the jawbone and preventing bone loss, thus maintaining the overall facial structure. 4. Improved Speech: Missing teeth can affect speech patterns and pronunciation. Dental implants fill the gaps and restore normal speech, allowing individuals to communicate clearly and confidently. 5. Convenience and Comfort: Dental implants eliminate the inconvenience and discomfort associated with removable dentures. Unlike dentures, which may slip or click during speaking or eating, implants remain securely in place, providing a comfortable and hassle-free experience. 6. Preservation of Adjacent Teeth: Traditional tooth-supported bridges require grinding down adjacent teeth for support. In contrast, dental implants do not rely on neighboring teeth for stability, preserving their natural structure and integrity. 7. Easy Maintenance: Dental implants can be cared for just like natural teeth. Regular brushing, flossing, and routine dental check-ups are all that is needed to maintain the health and longevity of implants. 8. Boosted Self-Confidence: The restoration of a complete and radiant smile can significantly enhance self-esteem and confidence. Dental implants provide a renewed sense of self, allowing individuals to smile, eat, and speak with confidence. 9. Improved Overall Quality of Life: Dental implants have a positive impact on overall quality of life. They restore oral function, improve appearance, and eliminate the self-consciousness often associated with missing teeth, enabling individuals to enjoy a more fulfilling and satisfying life. Read more: Advantages and Disadvantages of a Dental Implant FAQs about Dental Implants 1. Are dental implants suitable for everyone? No, not everyone is a candidate for dental implants. Certain medical conditions, such as uncontrolled diabetes or active gum disease, may affect the success of the implant procedure. It is essential to consult with a qualified dentist or oral surgeon to determine if you are a suitable candidate. 2. How long do dental implants last? With proper care and maintenance, dental implants can last a lifetime. However, individual factors such as oral hygiene practices and overall health can influence their longevity. Regular dental check-ups and good oral hygiene habits are crucial for ensuring the longevity of dental implants. 3. Is the dental implant procedure painful? The dental implant procedure is typically performed under local anesthesia, ensuring that patients experience minimal discomfort during the process. After the procedure, some mild soreness or swelling may occur, which can be managed with over-the-counter pain medication.  Introduction Having bleeding gums when flossing can be a frustrating and uncomfortable experience. However, it is a common issue that many people face. The good news is that there are several ways to address and resolve this problem. In this article, we will explore various methods to help you fix bleeding gums when flossing, ensuring a healthier oral hygiene routine. So, let's dive in and discover effective solutions to tackle this concern head-on. How Do You Fix Bleeding Gums When Flossing? Flossing is a crucial step in maintaining proper oral hygiene. However, if you notice bleeding gums during this process, it's essential to take action. Here are some effective strategies to fix bleeding gums when flossing: 1. Use the Right Technique: Proper flossing technique is vital to avoid irritating your gums. Gently guide the floss between your teeth, curving it against each tooth's surface. Be cautious not to snap the floss onto your gums, as this can cause injury. 2. Be Consistent: Regular flossing is key to preventing bleeding gums. Make it a habit to floss at least once a day, preferably before brushing your teeth. Consistency will help your gums adapt and become less prone to bleeding. 3. Choose the Right Floss: Not all flosses are created equal. Opt for soft and waxed floss to minimize gum irritation. Avoid using overly harsh or abrasive floss, as this can exacerbate the bleeding. 4. Don't Rush: Take your time when flossing and avoid rushing through the process. Being gentle and patient will allow you to clean your teeth effectively while minimizing trauma to your gums. 5. Rinse with Saltwater: After flossing, rinse your mouth with a warm saltwater solution. This natural remedy helps soothe irritated gums and promotes healing. 6. Consider Alternatives: If traditional flossing continues to cause bleeding, you may explore alternative methods such as water flossers or interdental brushes. These tools can be less abrasive on your gums while still effectively removing plaque and debris. 7. Maintain a Healthy Diet: A well-balanced diet rich in vitamins and minerals is essential for gum health. Include foods like leafy greens, fruits, and dairy products that provide the necessary nutrients for strong gums. 8. Stay Hydrated: Drinking an adequate amount of water throughout the day helps maintain saliva flow, which is crucial for healthy gums. Saliva neutralizes acids and removes food particles, reducing the risk of gum inflammation. 9. Quit Smoking: Smoking can greatly contribute to gum problems. If you're a smoker, quitting is not only beneficial for your overall health but also improves the condition of your gums. 10. Visit Your Dentist: If bleeding gums persist or worsen despite your efforts, it's crucial to consult a dentist. They can assess your oral health, identify any underlying issues, and provide appropriate treatment. Read more: Why do my gums bleed when I floss my teeth Frequently Asked Questions (FAQs) 1. Is it normal for gums to bleed when flossing? Occasional mild bleeding while flossing can be normal, especially if you've recently started or increased the frequency of flossing. However, persistent or excessive bleeding should be addressed. 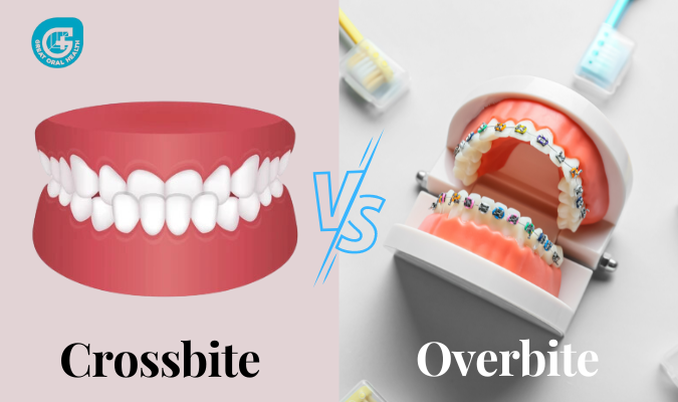 Introduction Dental misalignments can significantly impact oral health and overall well-being. Two common types of misalignments are Crossbite and overbite. While these terms might sound similar, they refer to distinct dental conditions. Understanding the difference between crossbite and overbite is essential for recognizing the symptoms, seeking appropriate treatment, and maintaining optimal oral health. In this article, we delve into the characteristics, causes, treatments. What is the Difference Between Crossbite and Overbite? Crossbite and overbite are both dental misalignments, but they affect the teeth and jaws in different ways. Here's a breakdown of their distinctions: 1. Crossbite: Teeth Misalignment Across the Jaw Crossbite occurs when one or more teeth are positioned closer to the cheek or tongue in relation to their corresponding teeth in the opposite jaw. In a crossbite, the upper teeth may sit inside the lower teeth when the jaws are closed. 2. Overbite: Vertical Overlap of the Upper and Lower Teeth Overbite, also known as "buck teeth" or "overjet," refers to the vertical overlap of the upper front teeth over the lower front teeth. In an overbite, the upper teeth protrude further forward than normal, causing an excessive vertical gap between the upper and lower teeth. Causes of Crossbite and Overbite Understanding the underlying causes of crossbite and overbite can help individuals identify potential risk factors and take appropriate preventive measures. The causes for each misalignment are as follows: Crossbite Causes
Read More: Effects of Crossbites Overbite Causes
Treatments for Crossbite and Overbite Both crossbite and overbite can be corrected with various treatment options, depending on the severity and individual needs. Here are some common treatments for each misalignment: Crossbite Treatments
Overbite Treatments
Frequently Asked Questions (FAQs) Can crossbite and overbite cause oral health problems? Yes, both crossbite and overbite can lead to oral health issues such as uneven tooth wear, jaw pain, temporomandibular joint (TMJ) disorders, and difficulty chewing and speaking. Can crossbite and overbite be fixed in adults? Yes, both crossbite and overbite can be corrected in adults. It's important to consult an orthodontist or a dental professional who can recommend suitable treatment options based on the individual's specific case.  Introduction When it comes to oral health, there's an age-old saying that goes, an apple a day keeps the dentist away. You've probably heard this adage at some point in your life, but have you ever wondered why people say it? Is there any truth to this popular saying, or is it just a myth passed down through generations? In this article, we will delve into the origins of this saying and explore whether there is any scientific basis to support the claim. So, let's bite into this topic and uncover the secrets behind why they say an apple a day keeps the dentist away. What Does an Apple a Day Keeps the Doctor Away Mean for Dentists? The timeless adage An apple a day keeps the doctor away emphasizes the importance of maintaining good health through preventive measures. While the saying doesn't explicitly mention dentists, it still holds true for dental health. When it comes to dentistry, the phrase implies that incorporating apples into your daily routine can help you avoid dental problems and maintain a healthy smile. Apples, with their natural properties, can serve as a simple and enjoyable addition to your oral care routine. Why Do They Say an Apple a Day Keeps the Dentist Away? It's time to get to the core of the matter and understand the reasons behind the saying An apple a day keeps the dentist away. While the saying may not be entirely accurate, it does hold some truth when it comes to maintaining good oral health. Let's explore the various factors that contribute to the dental benefits of consuming apples. 1. Natural Cleansing Action One of the primary reasons why apples are believed to be beneficial for dental health is their natural cleansing action. When you bite into an apple, its fibrous texture stimulates saliva production in your mouth. Saliva helps to neutralize harmful acids and wash away food particles and bacteria, reducing the risk of tooth decay and cavities. So, munching on an apple act as a natural toothbrush, keeping your pearly whites cleaner between brushing sessions. 2. High Water Content Apples have a high water content, which aids in maintaining oral hygiene. The water in apples dilutes the effects of sugar and stimulates saliva production, which helps to rinse away debris and maintain a healthy pH balance in the mouth. This can prevent the growth of bacteria and reduce the risk of dental issues such as plaque buildup, gum disease, and bad breath. 3. Vitamin C and Antioxidants Apples are a rich source of vitamin C and antioxidants, which are essential for gum health. Vitamin C helps in the production of collagen, a protein that strengthens gums and supports the connective tissues in your mouth. Antioxidants, on the other hand, help to protect your gums and other oral tissues from damage caused by harmful free radicals. By incorporating apples into your diet, you can provide your gums with the necessary nutrients to stay healthy and fight off infections. 4. Chewing Action Another aspect of why apples are beneficial for oral health lies in their crunchy texture. Chewing an apple stimulates blood circulation in your gums, promoting gum health. It also exercises the muscles in your mouth, keeping them strong and reducing the risk of tooth loss over time. So, the act of chewing apples can be considered a natural workout for your teeth and gums. 5. Low in Added Sugars Unlike many other sugary snacks and desserts, apples are relatively low in added sugars. High sugar consumption is one of the leading causes of tooth decay and cavities. By opting for apples as a healthy snack choice, you can satisfy your sweet tooth without exposing your teeth to excessive sugar. This, in turn, lowers the risk of dental problems and helps you maintain better oral hygiene. 6. Balanced Diet Eating an apple as part of a balanced diet contributes to overall health and well-being. A healthy body leads to a healthy mouth, and vice versa. By consuming a variety of nutritious foods, including apples, you provide your body with essential vitamins and minerals that support optimal dental health. Remember, good oral health is not just about brushing and flossing; it's also about nourishing your body with wholesome foods. Read More: Benefits of eating apples every day Conclusion The saying An apple a day keeps the dentist away may not be entirely accurate, but it holds some truth when it comes to maintaining good oral health. Apples contribute to oral hygiene through their natural cleansing action, high water content, vitamin C and antioxidants, chewing action, and low sugar content. However, it's important to remember that regular dental check-ups, along with proper brushing, flossing, and a balanced diet, are essential for maintaining optimal oral health. So, while enjoying the crispness and sweetness of apples, don't forget to schedule your next dental appointment to ensure a healthy smile.  Introduction Oral cancer is a serious and potentially life-threatening condition that affects various parts of the mouth, including the lips, tongue, cheeks, and throat. It is essential to be aware of the important points regarding oral cancer to ensure early detection, prompt treatment, and improved outcomes. This article aims to provide comprehensive information about oral cancer, including its causes, symptoms, risk factors, diagnosis, treatment options, prevention methods, and prognosis. Recognizing the Signs and Symptoms of Oral Cancer Oral cancer can present with a range of signs and symptoms, which can vary from person to person. It is crucial to pay attention to any unusual changes in the mouth and seek medical attention if any of the following symptoms persist:
If you notice any of these symptoms, it is important to consult a healthcare professional for further evaluation. Risk Factors for Oral Cancer Certain factors can increase the risk of developing oral cancer. Understanding these risk factors can help individuals take preventive measures and make informed lifestyle choices. The following are some common risk factors associated with oral cancer:
Diagnosis of Oral Cancer When oral cancer is suspected, a healthcare professional will perform a thorough examination and may recommend further tests for a definitive diagnosis. The diagnostic process may involve the following:
Treatment Options for Oral Cancer The treatment plan for oral cancer depends on various factors, including the stage of cancer, location, size, and overall health of the patient. The following treatment modalities are commonly used:
Preventive Measures for Oral Cancer Preventing oral cancer is essential for maintaining good oral health and overall well-being. While some risk factors for oral cancer, such as age and gender, cannot be controlled, there are several preventive measures individuals can take to reduce the risk. By adopting healthy habits and making conscious lifestyle choices, one can significantly lower the chances of developing oral cancer. Here are some preventive measures to consider: 1. Quit Smoking: Smoking is a major risk factor for oral cancer. By quitting smoking, individuals can greatly reduce their risk. Seek support from healthcare professionals or support groups to help with smoking cessation. 2. Maintain Good Oral Hygiene: Proper oral hygiene is crucial for oral health and can help reduce the risk of oral cancer. Brush your teeth twice a day, floss daily, and visit your dentist regularly for check-ups and cleanings. 3. Avoid Tobacco Products: In addition to smoking, other forms of tobacco use, such as chewing tobacco and snuff, also increase the risk of oral cancer. Avoiding these products altogether is crucial for oral health. 4. Limit Alcohol Consumption: Excessive alcohol consumption is strongly associated with oral cancer. It is advisable to limit alcohol intake or abstain from it altogether. Moderate drinking is defined as no more than one drink per day for women and two drinks per day for men. 5. Practice Sun Protection: Prolonged and unprotected exposure to sunlight increases the risk of lip cancer. To prevent this, use lip balms with SPF, wear wide-brimmed hats, and apply sunscreen to the face and lips when spending time outdoors. 6. Stay Hydrated: Adequate hydration is important for overall health, including oral health. Drink plenty of water throughout the day to keep your mouth moist and to help flush out harmful substances. 7. Eat a Healthy Diet: A balanced diet rich in fruits and vegetables provides essential nutrients and antioxidants that help protect against oral cancer. Include a variety of colorful fruits and vegetables in your daily meals. Read More: How to Accurate Is Oral Cancer Screening?  Introduction Being pregnant brings about numerous physical changes, and sometimes it includes experiencing a toothache. Hormonal fluctuations and changes in the body can contribute to dental discomfort. However, when seeking relief from a toothache during pregnancy, it is crucial to prioritize the safety of both the mother and the baby. In this article, we will explore the causes of toothache during pregnancy, discuss non-medicated and over-the-counter remedies, highlight medications to avoid and provide dental care tips for pregnant women. Causes of Toothache during Pregnancy During pregnancy, hormonal changes can lead to increased blood flow and fluid retention, which may affect the gums and teeth. The rise in hormone levels can make the gums more sensitive and susceptible to inflammation, causing gingivitis or exacerbating existing gum disease. Additionally, cravings for sugary foods or poor oral hygiene practices may contribute to tooth decay and cavities. Risks and Concerns While toothaches during pregnancy are common, it is essential to address them promptly to avoid potential risks and complications. Dental infections or abscesses left untreated can lead to more severe issues, including preterm birth or low birth weight. Hence, seeking appropriate dental care is crucial for maintaining oral health during pregnancy. Non-Medicated Remedies Fortunately, there are several non-medicated remedies that pregnant women can try to alleviate toothache discomfort: Cold Compress Applying a cold compress or ice pack to the cheek near the affected area can help numb the pain and reduce swelling. Wrap a few ice cubes in a thin cloth and hold it against the cheek for about 15 minutes. Take short breaks in between to prevent overexposure to cold. Over-the-Counter Options If the toothache persists or becomes more severe, pregnant women can consider over-the-counter options that are safe to use during pregnancy. However, it is crucial to consult with a healthcare professional or dentist before using any medications. Some common over-the-counter options include topical oral numbing gels or oral analgesics specifically designed for temporary toothache relief. Medications to Avoid During pregnancy, it is important to exercise caution when it comes to taking medications for toothache. Some medications can pose risks to the developing fetus. It is crucial to avoid the following medications without consulting a healthcare professional:
Always consult with a healthcare professional or dentist before taking any medication for a toothache at night during pregnancy. They can provide guidance on safe alternatives or prescribe suitable medications if necessary. Read More: When to Seek Professional Help While home remedies and over-the-counter options may provide temporary relief, it is essential to seek professional dental care if the toothache persists or worsens. Dental professionals can assess the underlying cause of the toothache and recommend appropriate treatment options that are safe for pregnant women. Delaying necessary dental care can lead to complications, so it is crucial to prioritize oral health during pregnancy. Dental Care Tips for Pregnant Women Maintaining good oral hygiene practices is vital for preventing toothaches and promoting overall oral health during pregnancy. Here are some dental care tips for pregnant women:
Read More: What Can You Do About a Toothache While Pregnant? Conclusion Toothaches during pregnancy can be uncomfortable, but there are safe and effective ways to manage the pain. Non-medicated remedies like saltwater rinses, cold compresses, and clove oil can provide temporary relief. However, it is important to consult with a healthcare professional or dentist before using any over-the-counter medications. Avoiding certain medications and seeking professional dental care when needed is crucial for protecting the health of both the mother and the baby. By practicing good oral hygiene and following the recommended dental care tips, pregnant women can maintain optimal oral health throughout their pregnancy journey.  A perfect smile is a combination of a healthy set of teeth and an aesthetically pleasing appearance. It is a crucial aspect of a person's physical appearance and contributes significantly to their self-confidence and overall well-being. But what exactly is the secret to a perfect smile? Let's dive deeper into this topic and explore the various factors that contribute to achieving a perfect smile. What is a perfect smile? A perfect smile is a smile that has a symmetrical appearance and is proportional to the face. The teeth are straight and evenly spaced, with no gaps or overlaps. The gums are healthy and are in proportion to the teeth. The color of the teeth is white and bright, without any discoloration or stains. The role of oral hygiene in achieving a perfect smile Oral hygiene plays a crucial role in achieving a perfect smile. Regular brushing and flossing help to remove plaque and prevent tooth decay, gum disease, and bad breath. It is recommended to brush at least twice a day for two minutes each time and floss once a day. In addition to brushing and flossing, it is essential to maintain good oral hygiene by visiting the dentist regularly for check-ups and cleanings. This will help to detect any dental problems early and prevent them from worsening. Poor oral hygiene can negatively impact a perfect smile, causing discoloration, tooth decay, and gum disease. Therefore, it is essential to establish good oral hygiene habits early on and maintain them throughout life. Diet and its Impact on the perfect smile A balanced diet is vital for maintaining good oral health and achieving a perfect smile. Foods rich in calcium and phosphorus, such as dairy products, leafy greens, and nuts, promote dental health and strengthen the teeth. On the other hand, sugary and acidic foods and drinks, such as candy, soda, and fruit juices, can harm dental health and lead to tooth decay and enamel erosion. It is important to limit the consumption of staining foods and drinks such as coffee, tea, and red wine to maintain white teeth. The Role of dental treatments in Achieving a perfect smile Dental treatments can also play a crucial role in achieving a perfect smile. Teeth whitening treatments can brighten the teeth and remove stains, while dental bonding can repair chipped or cracked teeth. Veneers can be used to correct gaps or misshapen teeth, and orthodontic treatments can straighten crooked teeth and correct bite issues. It is essential to consult with a dentist or orthodontist to determine which treatment option is best suited for your specific needs. Habits to avoid for a perfect smile There are certain habits that should be avoided to maintain a perfect smile. These include: 1. Smoking: Smoking not only harms overall health but also negatively affects oral health. It can cause staining, gum disease, and tooth loss, which can all impact the appearance of a smile. 2. Nail-biting: This habit can lead to chips or cracks in teeth and cause damage to the enamel, which can affect the appearance of a smile. 3. Chewing on hard objects: Chewing on hard objects such as ice, pens, or pencils can cause chips or cracks in teeth, which can affect the appearance of a smile. 4. Grinding teeth: Teeth grinding, also known as bruxism, can cause wear and tear on teeth, which can affect their appearance. It can also lead to jaw pain and headaches. By avoiding these habits, you can protect your teeth and maintain a perfect smile. Read More: The Power of a Perfect Smile Conclusion A perfect smile is a combination of healthy teeth and an aesthetically pleasing appearance. Achieving a perfect smile requires good oral hygiene, a balanced diet, and dental treatments when necessary. It is also essential to avoid habits that can harm dental health and the appearance of a smile. By prioritizing oral health and following these tips, anyone can achieve a perfect smile. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
June 2023
Categories |
 RSS Feed
RSS Feed
