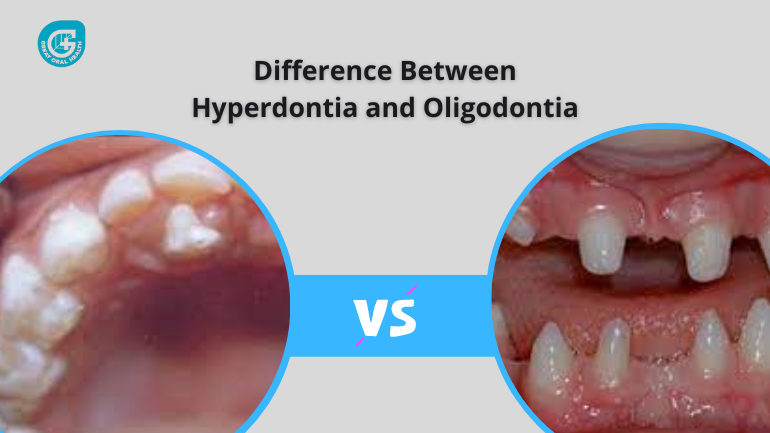
 Introduction When it comes to dental conditions, various terms might seem confusing. Two such conditions are hyperdontia and oligodontia. While they both pertain to the number of teeth, they are quite different in nature. Definition of Hyperdontia Hyperdontia, also known as supernumerary teeth, refers to the condition where an individual develops more teeth than the normal set. It is characterized by the presence of one or more additional teeth, which can appear in any area of the mouth. Symptoms of Hyperdontia The presence of supernumerary teeth may or may not cause noticeable symptoms. In some cases, the extra teeth may not erupt fully and remain impacted, leading to localized discomfort or pain. Hyperdontia can also cause overcrowding, misalignment, or malocclusion of the existing teeth. Diagnosis of Hyperdontia A thorough dental examination, including dental X-rays and imaging, is necessary to diagnose hyperdontia. X-rays can reveal the presence and position of the extra teeth. The dentist will assess the number, location, and impact of the supernumerary teeth to determine the appropriate treatment plan. Treatment for Hyperdontia The treatment approach for hyperdontia depends on the individual's specific case. In instances where the supernumerary teeth do not cause any problems, close monitoring may be sufficient. However, if the extra teeth are impacting oral health or causing aesthetic concerns, extraction may be recommended. Orthodontic treatment may also be necessary to correct any misalignment or crowding Caused by hyperdontia. Definition of Oligodontia On the other hand, oligodontia refers to the congenital absence of six or more permanent teeth, excluding the third molars (wisdom teeth). Individuals with oligodontia have a significantly reduced number of permanent teeth compared to normal dentition. Causes of Oligodontia Oligodontia can have both genetic and environmental causes. Genetic mutations or syndromes can lead to the absence of multiple permanent teeth. Environmental factors during tooth development, such as infections, trauma, or certain medications, can also contribute to oligodontia. Symptoms of Oligodontia The most obvious symptom of oligodontia is the absence of multiple permanent teeth. This condition can affect both the primary and permanent dentition. The missing teeth are usually incisors, premolars, or molars, and their absence can result in noticeable gaps or spaces in the mouth. Oligodontia can also lead to difficulties in chewing, speech problems, and a compromised aesthetic appearance of the smile. Diagnosis of Oligodontia The diagnosis of oligodontia involves a comprehensive dental examination, including a thorough evaluation of the patient's dental history and a physical examination of the oral cavity. Dental X-rays and imaging techniques, such as panoramic radiographs, can provide detailed information about the missing teeth and their impact on the surrounding dental structures. Genetic testing may also be conducted to identify any underlying genetic mutations or syndromes associated with oligodontia. Treatment for Oligodontia The treatment approach for oligodontia depends on various factors, including the number and location of the missing teeth, the overall oral health of the individual, and the patient's aesthetic concerns. The primary goal of treatment is to restore oral function, improve aesthetics, and promote long-term oral health. Read More: Different Types of Hyperdontia Treatment options for oligodontia may include: Prosthetic Replacement: Dental prosthetics, such as dentures or dental bridges, can be used to replace missing teeth and restore chewing function. These prosthetic appliances are custom-made to fit the patient's mouth and provide a natural-looking smile. Dental Implants: In cases where there are only a few missing teeth, Dental implants can be a viable option. Dental implants are artificial tooth roots that are surgically placed into the jawbone and serve as a stable foundation for dental crowns or bridges. They offer a long-term solution that closely resembles natural teeth in terms of appearance and functionality. Orthodontic Treatment: Orthodontic treatment, such as braces or aligners, may be necessary to correct any misalignment or malocclusion caused by the absence of multiple teeth. Orthodontic intervention can help optimize the alignment of the remaining teeth and improve overall oral function. Comprehensive Dental Care: Individuals with oligodontia require regular dental check-ups and preventive care to maintain their oral health. This includes professional cleanings, cavity prevention measures, and monitoring the condition of the existing teeth and supporting structures. Key Differences The key differences between hyperdontia and oligodontia can be summarized as follows: 1. Hyperdontia is characterized by the presence of extra teeth, while oligodontia involves the congenital absence of multiple permanent teeth. 2. Hyperdontia is associated with the development of supernumerary teeth, which can appear in any area of the mouth. In contrast, oligodontia primarily affects specific types of permanent teeth, such as incisors, premolars, or molars. 3. The causes of hyperdontia are not fully understood but may involve genetic factors or environmental influences during tooth development. Oligodontia can also have genetic causes, as well as environmental factors such as infections, trauma, or medications. 4. Symptoms of hyperdontia may include overcrowding, misalignment, or localized discomfort caused by impacted extra teeth. Oligodontia, on the other hand, is characterized by noticeable gaps or spaces in the mouth, difficulties in chewing, speech problems, and compromised aesthetics. 5. Treatment for hyperdontia may involve close monitoring, extraction of extra teeth if necessary, and orthodontic intervention to correct any misalignment. Oligodontia treatment options include prosthetic replacement with dentures or bridges, dental implants, orthodontic treatment, and comprehensive dental care.
0 Comments
 Introduction When it comes to dental health, we often hear the terms "plaque" and "calculus" being used interchangeably. However, they are not the same thing. Understanding the difference between plaque and calculus is crucial for maintaining good oral hygiene and preventing dental problems. In this article, we will explore the dissimilarities between plaque and calculus, their effects on oral health, and how to prevent and treat them. What is plaque? Plaque is a sticky, colorless film that forms on teeth. It is composed of bacteria, food particles, and saliva. Plaque accumulates on the tooth surface and along the gumline, particularly in areas that are difficult to clean, such as the spaces between teeth. The bacteria present in plaque produce acids that attack the tooth enamel, leading to tooth decay and cavities. Plaque is constantly forming in the mouth, and if not removed through proper oral hygiene practices, it can harden and develop into calculus. What is calculus? Calculus, also known as tartar, is a hardened form of plaque. It occurs when plaque remains on the teeth for an extended period, allowing minerals from saliva to deposit on it. Over time, this mineralization process causes the plaque to harden and transform into calculus. Unlike plaque, which is soft and can be easily removed by brushing and flossing, calculus is hard and firmly attached to the tooth surface. Its rough texture provides an ideal environment for bacteria to thrive, leading to gum disease and other oral health issues. Effects of Dental Plaque The accumulation of plaque on teeth can have detrimental effects on oral health. If not removed regularly, plaque can contribute to various dental problems, including: 1. Development of dental caries: The acids produced by plaque bacteria can erode the tooth enamel, leading to the formation of cavities or dental caries. Cavities, if left untreated, can progress and cause pain, infection, and even tooth loss. 2. Gingivitis and periodontal disease: Plaque buildup along the gumline can irritate the gums, leading to inflammation and gingivitis. If left untreated, gingivitis can progress to periodontal disease, which affects the supporting structures of the teeth, including the gums and jawbone. Read More: What Causes Plaque on Teeth? Effects of Dental Calculus Dental calculus, also known as tartar, is a hardened form of dental plaque that forms when plaque is not adequately removed from the teeth. Unlike plaque, which is soft and can be removed with proper oral hygiene practices, calculus requires professional intervention for removal. Here are some effects of dental calculus on oral health: 1. Consequences on Oral Health The presence of dental calculus can have several negative effects on oral health. As calculus accumulates on the teeth, it creates a rough surface that attracts more plaque, leading to further bacterial growth. This can exacerbate oral health problems and increase the risk of dental issues such as tooth decay and gum disease. 2. Calculus-Induced Gum Disease Dental calculus plays a significant role in the development and progression of gum disease. As calculus forms below the gumline, it creates a space between the teeth and gums, allowing bacteria to thrive. This can cause inflammation, redness, and swelling of the gums, leading to gum disease. If left untreated, gum disease can progress to periodontitis, which can result in tooth loss and damage to the supporting structures of the teeth. The differences between plaque and calculus While plaque and calculus are related, they differ in several key aspects:
It is important to note that both plaque and calculus contribute to the development of dental problems, and their removal is necessary to maintain optimal oral health. Read More: Difference Between Calculus and Cavity FAQs Q: Can plaque and calculus be completely prevented? A: While it is impossible to completely prevent plaque and calculus formation, practicing good oral hygiene, such as brushing twice a day, flossing daily, and visiting the dentist regularly, can significantly reduce their occurrence. Q: How can I remove plaque at home? A: To remove plaque at home, you should brush your teeth thoroughly for two minutes, twice a day, using a soft-bristled toothbrush and fluoride toothpaste. Additionally, flossing daily helps remove plaque from areas that a toothbrush cannot reach. Q: Can calculus be removed without professional dental cleaning? A: No, calculus cannot be effectively removed without professional dental cleaning. A dental hygienist or dentist uses special tools and techniques, such as scaling and root planing, to remove calculus from the teeth and gums. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
June 2023
Categories |
 RSS Feed
RSS Feed
